Although the United States is the richest country in the world we are lagging severely behind some third world countries in safe childbirth practices.
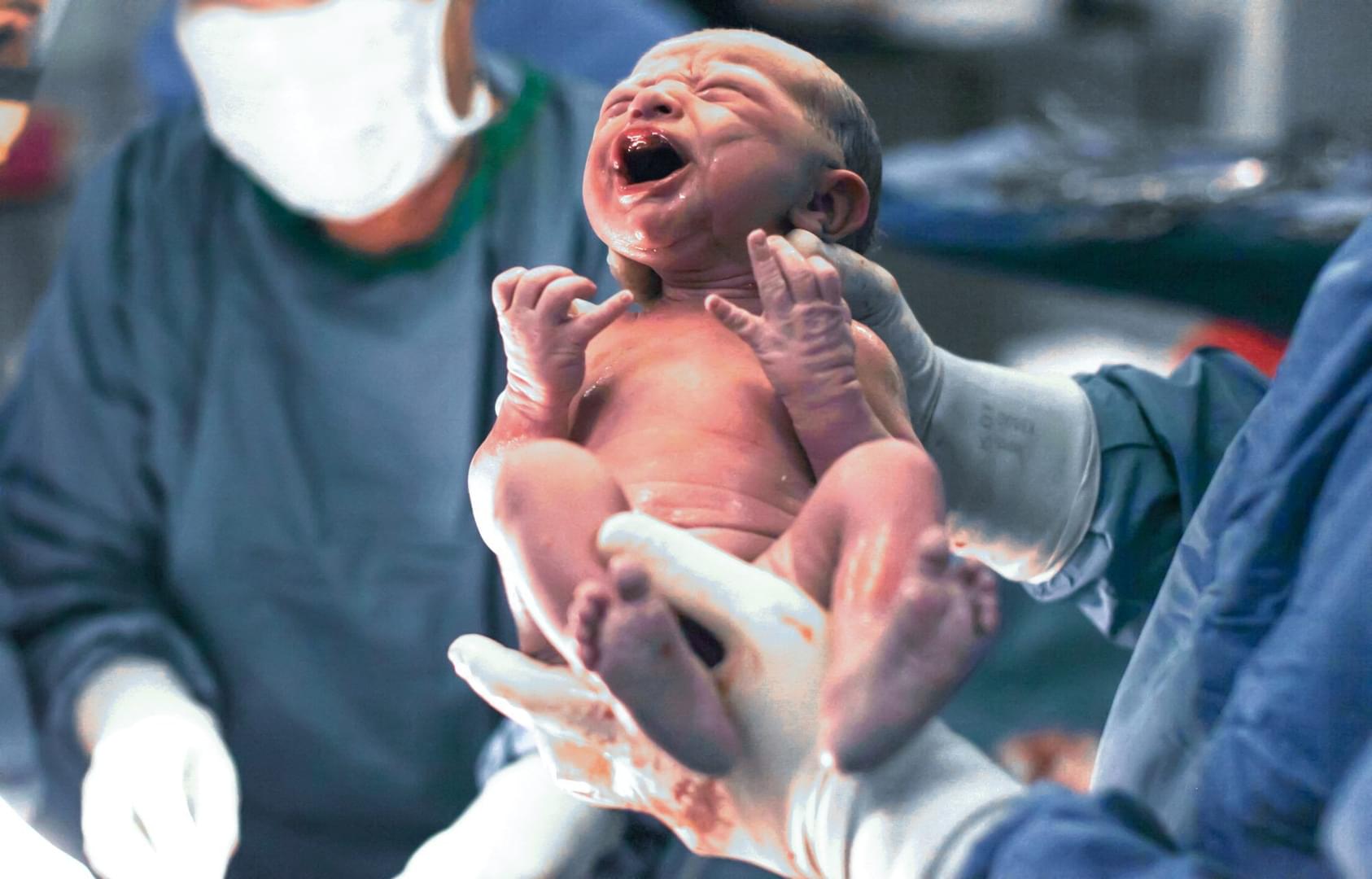 The birth of a child is a pivotal time in the life of a mother and her family. The health and well-being of a mother and child at birth largely determines the future health and wellness of the entire family. The outcome of childbirth, however, is not the only factor of importance in a mother’s well-being. Some research suggests that the way in which a woman experiences pregnancy and childbirth is also vitally important for a mother’s relationship with her child and her future childbearing experiences.
The birth of a child is a pivotal time in the life of a mother and her family. The health and well-being of a mother and child at birth largely determines the future health and wellness of the entire family. The outcome of childbirth, however, is not the only factor of importance in a mother’s well-being. Some research suggests that the way in which a woman experiences pregnancy and childbirth is also vitally important for a mother’s relationship with her child and her future childbearing experiences.
In preparing to give birth, women, knowingly or unknowingly, develop a birth plan. The use of formal birth plans developed in the 1980s as a way for women to engage in discussion with their care providers and to articulate their desired birth experience. Birth plans generally include information such as where a woman wishes to give birth, who will attend a birth, and what forms of medical intervention and pain relief will be used. The birth plan is a tool that outlines a woman’s expectations for her birth and can open communication between a woman and her care providers, providing the woman with knowledge prior to giving birth. There may also be negative outcomes of developing a birth plan; for example, feelings of failure if the birth plan is not followed and disappointment with the birth experience if expectations are not met.
The birth plan is a tool that outlines a woman’s expectations for her birth and can open communication between a woman and her care providers, providing the woman with knowledge prior to giving birth.
When negotiating birth plan decisions, women tend to alter their expectations to avoid disappointment. When expectations are altered, the care providers and support team become vitally important in helping to negotiate changes and foster a positive birth experience. For the purposes of this study, we defined a woman’s “care team” or “support team” as all individuals who assist with planning and giving birth, including obstetricians, midwives, nurses, doulas, friends, family members, and the woman’s partner, all of whom may shape a woman’s thinking about planning a birth.
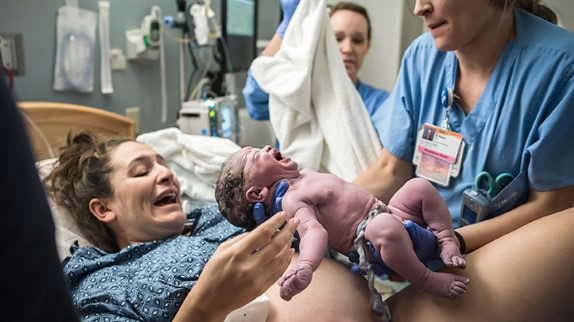
There is a constant negotiation of expectations and desires for the birth between a woman and her support team. During both the development and implementation of the birth plan, women must negotiate their expectations and make health decisions with their care providers. The role of the care provider is central in the ways in which women make decisions.
When women are well supported in making decisions and have a great deal of trust in their care providers to make decisions on their behalf, women have a more positive recollection of their birth experiences.
The connection between control over birth plan and overall view of the birth process is consistent with the findings of a studies that concluded that control over the physical, emotional, and mental aspects of childbirth are important to women.
Women who were supported with consultation from their entire care team and family, related to changes in their birth plans, did not experience a severe loss of control. Women who do not have that opportunity to be consulted experience a greater loss of control and, therefore, describe a more negative overall experience.
All members of the labor and birthing care team, including family, partners, nurses, doulas, midwives, and obstetricians, need to support women in making informed choices and negotiating these decisions during the birth process.
What choices you make in your family's birthing process can affect you for the rest of your life. The Patient Advocacy Group can help guide you through the healthcare process and allow you to confidently make the right decisions for what is best for you. Whether you decide to go the traditional birthing process, a medication-free birth, a home birth, a birthing center, or a Doula or Midwife, we will help explain your options and evaluate your insurance limitations and find the professionals to help you experience the safest experience possible.
Our role is to help people with PRENATAL and POSTNATAL care — ensuring their questions are answered, concerns are heard, and wishes are respected. Such care may involve scheduled induction, scheduled c-sections, alternatives to gestational diabetes testing, retesting group B strep before due date, declining tests/vaccines/interventions, informed consent, and refusal of cervical checks.
For postnatal, making sure their wishes for their baby are honored — i.e. eye ointment, vitamin K and hepatitis B, golden hour, breastfeeding/formula feeding, baby in nursery or in room, etc. Also, at their 6-week check-in — are their concerns being heard? Is doctor thoroughly making sure the mother is ok or just checking off boxes?